23 October 2023
AusHealth Research Congratulates Professor Glenn King: A Remarkable Journey from Spider Venom to Groundbreaking Therapeutics.
General
Research
AusHealth, a leading healthcare innovation company, is delighted to extend its warmest congratulations to Professor Glenn King for his exceptional contributions to the field of biomedicine and winning the 2023 Prime Minister's Prize for Innovation.

12 October 2023
Medvet Oral 7 & RapidScreen Saliva 7
General
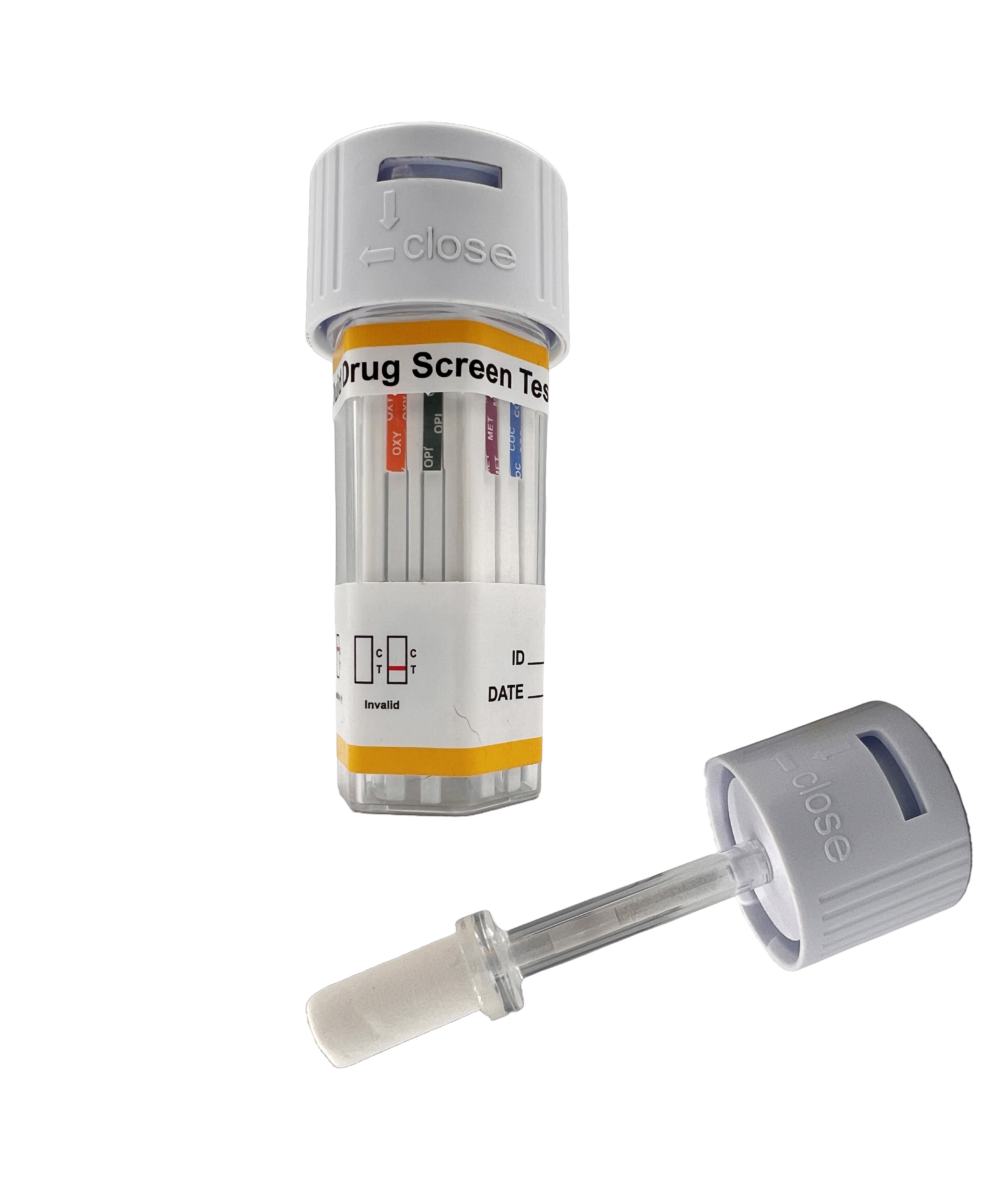
The Medvet Oral 7® & RapidScreen Saliva 7® is the leading oral testing device in Australia. It has been verified to detect seven commonly abused drugs and their by-products in human oral fluid to meet the Australian Standard.
Oral fluid drug testing is now a convenient and reliable alternative to urine drug testing. It allows for easy and repeated collection of oral fluid samples in various situations.
Oral fluid drug testing is now a convenient and reliable alternative to urine drug testing. It allows for easy and repeated collection of oral fluid samples in various situations.
5 July 2023
AusHealth is now a registered health charity
Research
As of July 1, 2023 AusHealth is now a registered charity, furthering our ability to pioneer medical research for a healthier tomorrow.

24 May 2023
Is Alcohol Affecting Your Workplace?
General
Drug and alcohol use in the workplace comes with a significant financial cost to businesses.

23 January 2023
Should I get a flu vaccination this year?
Work
2023 is gearing up to be a more challenging year for flu cases than the pandemic. Here's why you should book in for a flu vaccination.

14 November 2022
Diabetes research inspired by Australia's native wildlife
Research
AusHealth Research has discovered a new way to treat diabetes, inspired by the mating habits of Australia's native wildlife.

13 September 2023
R U OK - I'm here to hear
General
R U OK? Day – September 14, 2023. As we mark another 'R U OK? Day', it's a crucial reminder that sometimes a simple conversation can make a world of difference. We all face challenges, moments of self-doubt, and personal struggles, but by reaching out and asking, "R U OK?", we can bridge the distance between isolation and connection.

15 June 2023
Managing Mental Health for Well-being and Success in the Workplace
Work
Learn effective strategies to manage mental health through AusHealth's range of wellness courses for workplace relations.